If the future is as bright as we believe it will be, regarding the use of naturally-occurring bacteriophages to kill Borrelia, and the co-infections common in the tick-borne diseases, such as Lyme disease, the fear of causing a severe Jarisch-Herxheimer response (JHR), may become a thing of the past.
A Jarisch-Herxheimer response, otherwise known as a Herx reaction is a worsening of person’s symptoms associated with immune cells in the body releasing cytokines that increase inflammation. The popular idea that a herx is due to the direct die off toxins of the bacteria is not supported by the latest research. This article will present research as to why bacteriophage killing of bacteria do not result in severe herx reactions when compared to antibiotic use, and present preventive measures to minimize herx reactions.
It is common to see the complete annihilation of the Borrelia population within one week with effective bacteriophage therapy, combined with support from the innate immune system, primarily neutrophils. While this time frame is much quicker than any known antibiotic treatment, which often requires weeks to years of multiple antibiotics, it does necessitate comprehensive measures be taken to avoid even minor herx reactions.
What Causes a Herx?
In order to develop effective therapeutic countermeasures to herx reactions, the pathophysiology, or the disordered physiological processes associated with a herx reaction, must be understood.
Many authors have proposed that the herx is caused by the release of toxins by dying spirochetes, hypersensitivity to spirochetes, removal of dead spirochetes by phagocytic cells, complement activation, DIC, and mediators of inflammation including cytokines and histamine. However, according to the most recent understanding, many of these mechanisms are unsupported and probably wrong.
In a review of the research, Thomas Butler states, “After antibiotic treatment, spirochetes are rendered more susceptible to PMN phagocytosis likely caused by an alteration of the microbial surface to expose antigens and molecular patterns that allow antibody and complement to bind more effectively for phagocytic uptake. Once inside, PMN spirochetes probably provoke more severe inflammation.”
Butler goes on to say, “Causes of inflammation in the JHR are multifactorial. When spirochetes are cleared from blood by phagocytosis, rises in concentrations of pro-inflammatory cytokines occur. Spirochetal inflammatory substances include lipoproteins and nonendotoxin pyrogens that cause rises in cytokines such as TNF-a, IL-6, and IL-8, as well as rises in histamine.”
Less Herx From Bacteriophages Than Antibiotics:
Bacteriophages kill bacteria by a process called lysis, the disintegration of the bacteria by rupture of the cell wall or membrane. To see this in action, watch the National Institute of Health video on this link. Research has demonstrated that Borrelia burgdorferi which were killed by lysis, did not cause nearly as much cytokine release, or inflammosomes. Conversely, antibiotics often cause increased phagocytosis of the bacteria, resulting in significantly greater transcription of proinflammatory cytokine genes than do lysates.
Anti-Herx Therapeutic Measures:
- Botanical/Nutitional/Homeopathic/Fatty Acid: anti-inflammatory and anti-cytokine support
- I.V. Hydration has been shown to reduce the occurrence and severity of herx reactions
- Hyperbaric Oxygen therapy (HBOT), and other oxygen therapies have been shown to reduce the severity of herx reactions
- BEMER mat therapy
- Near/Mid/Far Infrared Sauna therapy
- Antihistamines and enhance optimum histamine clearance via enzyme activation in the metabolic pathway.
- NSAID’s can have a beneficial effect on acute herx reactions
Summary:
Physicians need to anticipate a JHR when treating spirochetal diseases to provide supportive care of monitoring vital signs and administering fluids. The prognosis is favorable for full recovery even if a herx reaction occurs, usually resolving in a few hours in most patients given supportive care and adequate fluid.
Although for many years it was thought that a Herxheimer reaction was caused by the toxins released as bacteria die and break apart, we now know this is incorrect. A Herxheimer reaction the result of the ingesting of the live, antibiotic-weakened bacteria, by immune cells, specifically polymorphonuclear leukocytes, white blood cells, such as neutrophils, which eat the live bacteria and eventually digest them, but in the meantime the bacteria, through genetic transcription cause the production of highly proinflammatory cytokines, TNF-a, IL-6, IL-8, and histamine.
When the target bacteria die from lysis, as is the case with bacteriophage therapy, the bacteria burst and the polymorphonuclear cells gobble up the dead pieces. In that there are no live bacteria essentially being eaten by these immune cells, very little cytokines are produced.
In that bacteriophages kill extremely quickly, killing all of the target bacterial population usually in less than seven days, which means that by the time the immune system can begin to respond, the war is over. Not only that but because of the way that the bacteriophages kill the bacteria, via lysis, meaning the bacteria are broken apart where they sit. This means when neutrophils gobble up the bacterial pieces, that no live bacteria are being eaten, therefore the bacteria cannot cause genetic transcription thus cannot cause the production of excessive proinflammatory cytokine substances. All of this translates into much less herx symptoms than do antibiotics.
Conversely, many of the worsening symptoms experienced with antibiotics, and even with the latest trending antibiotic, Disulfiram, are due to the disruptive nature on the patient’s metabolic processes and frank antibiotic sensitivities. These antibiotic-induced herx symptoms are often the cause of poor patient compliance, often causing the patient to self-reduce the therapeutic dosage, enabling improved tolerance but greater risk of bacterial mutations rendering the drug ineffective. Antibiotic treatment can also result in new symptoms that can last months or be permanent.
Bacteriophage therapies are a superior form of treatment in the fight of treatment-resistant microbial infections.
Learn more about the potential for Induced Native Phage Therapy (INPT) at the Biologix Center for Optimum Health, in Franklin, Tennessee.
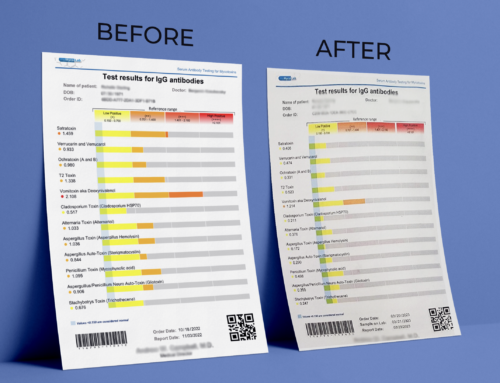
Learn more about using Borrelia-phages in a much more accurate lab test to diagnose Lyme disease. Available at the Biologix Center.